Social Distancing Is Here to Stay, So The Time Has Come for Telemedicine
Just ask any doctor: there is always a risk of contagion when visiting a medical center. Telemedicine is how you dramatically cut down that risk.
Numberless academic studies have proven that telemedicine has multiple advantages over face-to-face consultations. It allows for faster diagnosis and treatment; facilitates patient follow-up; prevents transfers; can improve the services provided; and favors teamwork between the different professionals involved, fostering inter-consultations and motivating easier access to second opinions.
There's more. It also helps to shorten waiting times, assists in making appointments, and facilitates patient-doctor communication in general; it can reduce inequalities in accessibility; and it is more cost-effective than building medical units or moving teams of specialists to remote areas that require support.
The danger of COVID-19 infection in health centers – which is similar to that faced in many everyday situations – should not be underestimated. Yet it is clear that telemedicine has many advantages, so the question is obvious: why don't we use telemedicine more often?
The answer is anything but simple since every country in Latin America and the Caribbean (LAC) has different barriers when it comes to effectively implementing this technology.
First, there is a need to review each government’s adaptive capacity. Obsolete regulatory frameworks that fail to adapt to the new digital reality often prevent the use of private telemedicine initiatives that can prove extremely beneficial, especially for isolated communities or those with limited access to hospitals and medicines.
A first step to reducing the health gap through technology should be to review and develop regulatory frameworks for the online provision of medical services and sale of pharmaceutical products.
Second, there are several relevant material barriers, such as a lack of investment in suitable equipment and difficulties to access communication networks, which bogs down the development of telemedicine and other advances in medical technology. According to the latest Broadband Development Index (iDBA), LAC lags significantly there behind compared to the most advanced OECD countries due to worse broadband adoption, affordability, and coverage rates, which must be improved.
Third, there is a pressing urge to train medical personnel in new technological advances. Remote diagnostics and treatments, or even remote surgeries – such as those performed by Dr. Antonio de Lacy at the World Mobile Congress in 2019 – are a new reality that, despite optimizing medical professionals’ time availability, require different training and preparation methods than those used so far. Health professionals’ training must therefore be improved.
Fund distribution is key: as the pandemic continues to shake global markets, private equity funds have doubled their investments in healthcare companies in emerging markets. According to EMPEA, an association that brings together private investors in emerging markets, total capital invested in the health sector saw a 52% year-on-year growth, reaching a record US$9.9 billion in the first half of 2020. These resources must be used smartly.
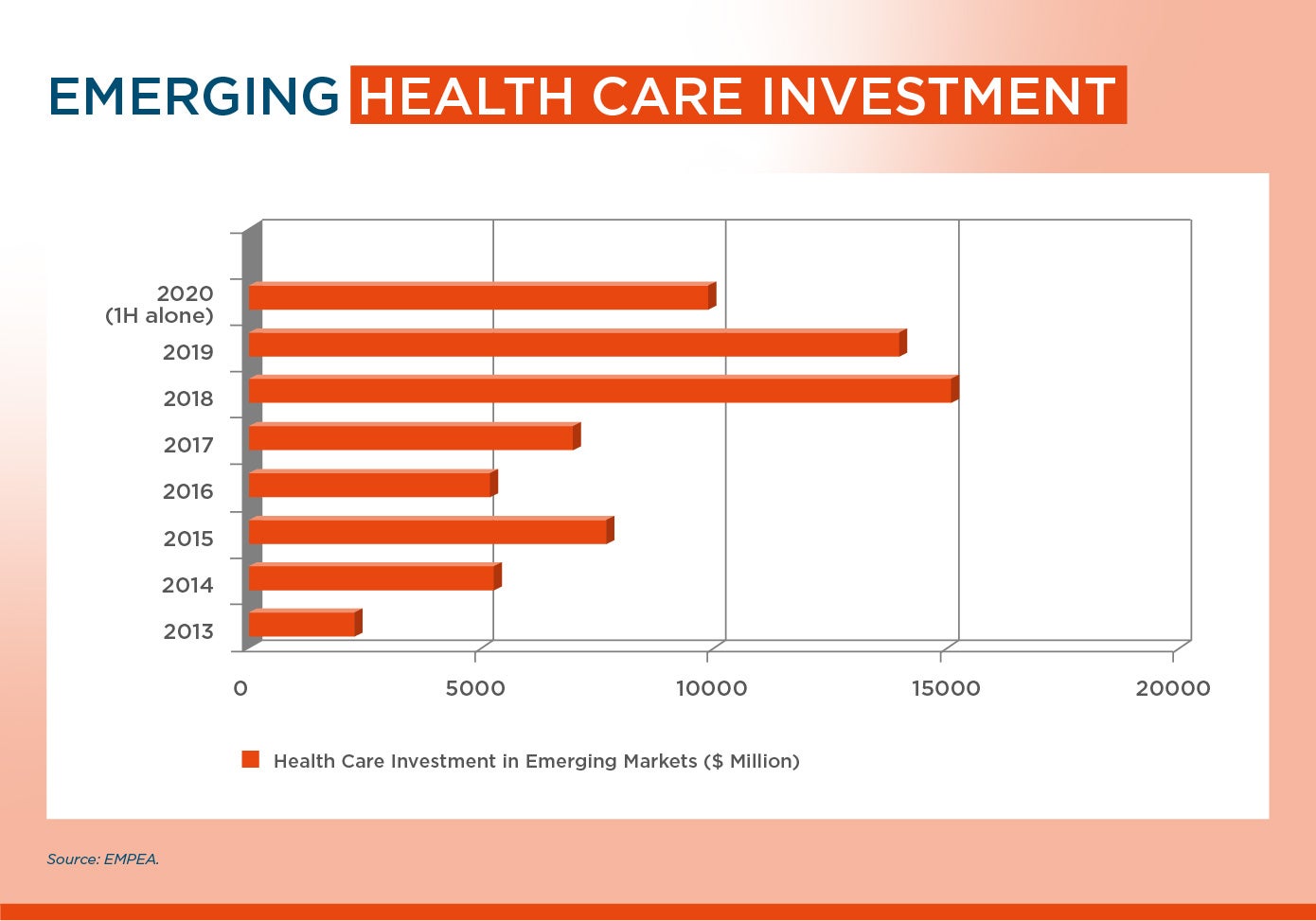
The resources destined for telemedicine must coexist with sustained investment in physical infrastructure and equipment, as well as research. These factors remain vital for improving health services management and are key in the context of a pandemic.
A good example is the case of the Albert Einstein Hospital in Sao Paulo, a key player during the pandemic due to its ability to adapt to a highly complex scenario – such as the one confronted by the Brazilian state early on. Its response plan, financed by IDB Invest, allowed it to add 528 beds to the public health system, reaching a total capacity of 951 beds for COVID-19 patients, 108 beds for the Intensive Care Unit (ICU), and 49 hospitalization beds for its private branch.
COVID-19 has boosted the digital industry, and technology is here to stay. The pandemic is a driver for many great innovations, particularly in areas such as remote healthcare or home hospitals, or the sense of urgency in thinking about how to care for the elderly. These innovations are not going to disappear, since pandemics are no longer rare occurrences. The H1N1 pandemic took place in 2009, and 2020 saw COVID-19; it is highly probable that there will be other such pandemics in the coming years. We must learn from the past and prepare for the future.
LIKE WHAT YOU JUST READ?
Subscribe to our mailing list to stay informed on the latest IDB Invest news, blog posts, upcoming events, and to learn more about specific areas of interest.
Subscribe



